 Objectives Objectives
1. Describe the reasons abortion at less than six weeks gestation was impractical in the 1970�s. What advances in technology have not made it practical.
2. Explain the concept of �discriminatory zone� and its implications for providing medical abortion, early surgical abortion and detecting ectopic pregnancy.
3. Discuss the benefits of surgical abortion at less than six weeks to the patient, to the physician and to the staff.
4. Discuss the skills and services needed to provide medical abortion.
5. Understand the pitfalls of relying only on pathologic examination of curettings to confirm the removal of an intrauterine pregnancy.
 History of Early Surgical Abortion History of Early Surgical Abortion
After
abortion became widespread in the United States in the early 1970s, technical
limitations to very early (less than six gestational weeks) surgical abortion
became evident. Pregnancy tests commercially available at that time detected
levels of human chorionic gonadotropin (hCG) of 1500-2000 IU/L (first
International Reference Preparation) making it impossible, outside of a research
setting, to confirm a pregnancy before six weeks gestation. Moreover, clinicians
found it difficult to visually confirm the presence of products of conception in
the surgical specimen and pathological examination often failed to identify
villi. Most retrospective studies
of abortion complications indicated an much higher risk of complications such as
febrile morbidity, hemorrhage requiring blood transfusion and unintended major
surgery for gestations of less than six[i],[ii]
During the last 15 years technological advances such as vaginal ultrasound,
high-sensitivity urine pregnancy tests, and readily available serum b-hCG tests have moved the
diagnosis of normal and ectopic pregnancy well within the first six gestational
weeks.[iii]
This technology also allows
very early pregnancy termination.
The availability of home pregnancy tests for less than ten dollars that
are positive as soon as eight days after conception has created patient demand
for early pregnancy termination.[iv]
Most women who have made a decision to terminate a pregnancy
wish to have the abortion done as soon as possible as long as there is no
additional risk. Our study of 2,400
cases has shown that pregnancies less than 6 weeks gestation can be safely
terminated using manual vacuum aspiration. The use of a
hand-held vacuum syringe with a 7 mm rigid cannula combined with pre and post
operative vaginal ultrasound to demonstrate complete aspiration is a safe and
effective technique for early abortion. The
surgical technique is only slightly more difficult than that of endometrial
biopsy. If the observation of
chorionic membrane and villi do not confirm a complete abortion, follow up with
serum b-hCG
is required. This approach has the additional advantage of quickly detecting
unsuspected ectopic pregnancy.
 Ultrasound in Early Surgical Abortion Ultrasound in Early Surgical Abortion
Ultrasound
is used to date the early pregnancy and to confirm the removal of the
gestational sac and the decidua. The
approximate gestational age can be determined because of the sequential
appearance of the embryonic structures. When
there is no gestational sac by vaginal ultrasound and the pregnancy test is
positive, the gestation is 3 weeks (LMP) or is an ectopic pregnancy.
When there is a gestational sac visualized the pregnancy is 4 weeks or
(rarely) an ectopic pregnancy with a pseudosac.
When the gestational sac and yoke sac are visualized but there is no
fetal pole the gestation is 5 weeks.[v]
Alternately
the gestational sac diameter can be measured and the gestational age determined
by the average diameter of the sac. The formula to calculate the gestational age
is:
Gestational
age (days)=mean sac diameter (mm) + 30
The
ultrasound is also useful for detecting abnormal anatomy (fibroids, uterine
septa) that might complicate the abortion procedure.
 Surgical Procedure Surgical Procedure
Two
models of hand held syringes of slightly different design are available in North
America. The IPAS*
syringe has a valve that allows the vacuum to be created prior to inserting
the cannula into the uterus. The
Milex syringe has a locking plunger that prevents inadvertent loss of pressure
during the procedure but the vacuum must be created after the cannula is inside
the uterus. I will describe the use of the IPAS syringe although the
Milex can be used with minor modification.
The
abortion procedure is exactly the same as other first trimester procedures up to
insertion of the cannula through the cervical os. The use of local anesthesia,
conscious IV sedation, general anesthesia and other adjuncts will not be
described in this text. The 7 mm
cannula is firmly seated into the opening of the syringe.
The valves are then closed and the plunger is extended (pulled out) to
create a vacuum. The cannula is
then inserted with a twisting motion through the cervix, which has been dilated,
to a 21 French circumference using tapered (Pratt) dilators. The valves are then
released and the uterine contents removed with both rotation and back and forth
movements. Often the white gestational tissue can be seen passing through the
cannula. When the uterus is felt to
be empty the cannula is removed. When
the cannula tip is removed from the uterus a rush of air can be heard assuring
that the vacuum has been maintained during the procedure. A vaginal ultrasound
examination of the uterine cavity while the patient is still on the examination
table confirms the removal of the gestational sac and decidua.
When the OR does not have a readily accessible ultrasound machine the
post op ultrasound can be limited to only those cases in which appropriate
membranes and villi are not seen in the curettings.
The use of the hand held syringe and the large bore (7 mm) cannula allows
the gestational membranes and villi to be removed relatively intact. The gestational tissue is then easy to identify with thorough
washing and floating in a backlit dish. In
those cases in which definite gestational membranes and villi are not
identified, blood is drawn for an immediate
b-hCG. In our
experience gestational tissue is not identified in about one case out of every
20 under six week gestations or in about 50% of gestations in which the
gestational sac is not seen on vaginal ultrasound. The cost of the b-hCG
testing is far outweighed by the benefit to the patient of early identification
of unsuspected ectopic pregnancy and the convenience of an early procedure.[vi]
When
the b-hCG is drawn it is necessary to use a specific follow up protocol.
If the initial b-hCG is above that of the laboratory�s discriminatory zone the
patient must be
sent
for immediate evaluation of a possible ectopic pregnancy. If the initial b-hCG
is less than the lab�s discriminatory zone a follow up b-hCG must be drawn in 24-72
hours. If the level fails to drop
by at least 50% in the second study the patient must be evaluated for possible
ectopic pregnancy. Most of the ectopic pregnancies detected by this method are
suitable for treatment with methotrexate, thereby avoiding a surgical procedure.*
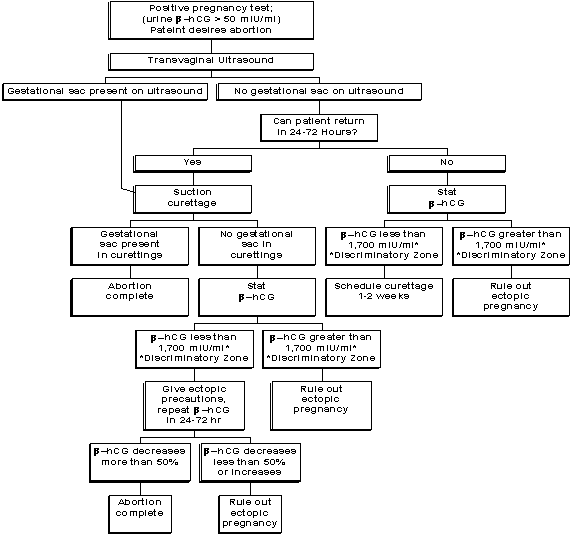
 Algorithm for Abortion at Less Than Six Weeks
Gestation Algorithm for Abortion at Less Than Six Weeks
Gestation
 Examination of the Products of Conception Examination of the Products of Conception
An
integral part of any surgical abortion procedure is the examination of the
products of conception. The
surgical procedure is not complete until the surgeon has examined and
ascertained that the products of conception are complete and correlate with the
gestational age. Many of the
delayed complications of abortion will be minimized when complete removal of the
appropriate amount of gestational tissue is confirmed by a systematic
examination of the tissue by the clinician. Physicians performing first
trimester abortions will inevitably encounter patients whose pregnancies are
ectopic but who have not yet experienced symptoms typical of more advanced
ectopic pregnancies. A formal, microscopic examination of the tissue by a
pathologist, while useful in screening for molar pregnancy, does not reliably
provide the most relevant clinical information.
Other reasons for pathological examination include requirements by state
laws and as a means of disposal of aspirated tissue. The clinician should
confirm not only that gestational tissues (membranes, villi, fetal parts) are
present but also that the amount of tissue is consistent with the gestational
age. A pathological examination can be signed out as �positive for
trophoblastic tissue� when the main portion of the pregnancy remains in the
uterus or is a cornual or tubal ectopic pregnancy, It is common for
the pathologist to fail to detect a small 3 or 4 week gestational sac because of
the relatively large amount of decidual tissue. Careful examination of aspirated
tissue is the key to early diagnosis of ectopic pregnancy and is the
responsibility of the physician who has performed an abortion.
 Discriminatory zone and detection of ectopic pregnancy Discriminatory zone and detection of ectopic pregnancy
For
the clinician to implement this protocol, it is necessary to understand the
concepts underlying the modern detection of ectopic pregnancy.
The concept of a discriminatory hCG zone was introduced Kadar in 1981.[i]
The discriminatory zone is defined as that level of hCG at which a intrauterine
pregnancy should always be seen on ultrasound. The original concept was of
little use in management of ectopic pregnancies since it was formulated using
abdominal ultrasound. The required hCG level of 6500 IU/L (second International
Reference Preparation) was present at initial presentation in less than 10% of
patients with ectopic pregnancies. The concept was adapted for the more
sensitive (5-10 MHz) endovaginal transducer by Bernaschek[ii]
and others; the discriminatory zone was in the 1000 to 2000 IU/L range and,
therefore, much more useful since this level was usually present by the time the
ectopic pregnancy became symptomatic.
3
Although
many clinicians now require the visualization of a gestational sac on vaginal
ultrasound before performing a surgical abortion, the experience with the
protocol described here demonstrates that such visualization is not necessary.
Goldstein first proposed that visualization of a gestational sac is not a
necessary prerequisite for a pregnancy termination if the patient is followed
closely by �-hCG measurements.[iii]
Such "biochemical visualization" assures that the pregnancy is
terminated. In his series of 21 patients with no gestational sac on endovaginal
scan, 17 (81%) had villi by gross or microscopic exam. The described here uses
modified gross exam (3X magnification) since microscopic tissue reports are not
immediately available and are often misleading. Kadar, following a similar
protocol (albeit with abdominal ultrasound), recommended against doing a
curettage when the gestational sac was not seen.
7
His
protocol required the patient to return in a week for further evaluation and
curettage; this extra week, if an ectopic pregnancy is present, could result in
serious consequences. Also patients may not be able to return or may be lost to
follow up. In our study seven out of fourteen of our patients with ectopic
pregnancies had their diagnosis made and treatment begun the day they came for
their abortion. Of the 242 patients with a 3 week (21 to 27 day) gestation, 51%
went home the day of surgery with assurance that their pregnancy was terminated
and that no further evaluation (other than routine follow up) was needed. Had
the recommendation of Kadar been followed, all 242 patients would have had to
return in one week and 13 (5.4%) women would have had a delay in the diagnosis
of their ectopic pregnancy.
 Costs of the protocol Costs of the protocol
It
is important to understand the necessary costs of establishing this protocol as
part of clinical abortion practice. Minor costs include a manual vacuum
aspiration syringe and a fluorescent magnifying lens. A potential major expense
could be an ultrasound machine with a vaginal transducer. However, many ob/gyn
physicians already have an ultrasound machine in the office or clinic; thus, the
need for an ultrasound machine is not likely to result in any additional cost.
Extra staff time will be needed to contact patients who do not return as
scheduled, follow-up on laboratory results, and explain the extra instructions
sometimes necessary for these patients. The most notable extra cost is the
quantitative �-hCG tests. Still, a relatively small number of the 2399 patients
required follow-up �-hCG evaluation. Only 283 hCG tests were required to
evaluate the 125 patients in whom no gestational sac was seen in the curettage
specimen at a total cost of $9905 ($35.00 per test.) This cost averages to
$79.20 per patient for those with no gestational sac visualized but, when
apportioned among the entire patient population, is only $4.13 per patient. The
average cost of �-hCG evaluation to find an ectopic pregnancy was $707.50
($9905 and 14 ectopic pregnancies.)The direct cost of surgical treatment of
ectopic pregnancy has been estimated at $8000 and $9482 and the direct costs of
MTX treatment of ectopic pregnancy at $670.[iv]
Since the ectopic pregnancies in this series were diagnosed very early in
gestation, this protocol may potentially increase the number of women eligible
for medical rather than surgical treatment. Also, there is less potential for
tubal damage when the ectopic pregnancy is diagnosed 1-3 weeks before clinical
symptom. It is possible that this protocol incurs unnecessary expense and
instrumentation in women who would have otherwise had an early spontaneous
abortion and not required medical care or surgical intervention.
 Starting to provide early surgical abortions Starting to provide early surgical abortions
For
those planning to offer early abortion procedures it is important to Adopt
the whole package!
Adhere to the protocol by using the correct instruments and following the
algorithm. The high efficacy and
low complications will not be achieved if you adapt, pick and choose from the
methodology. Wait until after your
first 1,000 cases to try a different idea.
Order the film (Surgical Abortion Before Six Weeks Gestation) and review
it with your staff. A
knowledgeable, well informed staff will be your greatest asset both in informing
and reassuring the patients and in making sure there is good follow up. The
belief that early abortion is more painful and fraught with risk of failure and
complications is deeply ingrained in the psyche of your staff, the medical
community and the general public. Your
staff will create a self-fulfilling prophecy if they tell patients that it will
be more painful. You must make sure
that receptionist, nurses, counselors, volunteers, and administrative staff know
about the procedure.
Common mistakes in
starting the protocol:
I�ll
just turn the suction down on the machine, that should be just as good as using
the hand held suction.
I�ll
use the small, soft Karmann cannula. Don�t
you need a small cannula for a small pregnancy?
I�ll
not worry about examining the tissue because we are going to send it for
pathology and pathologist are the experts at identifying gestational tissue.
I�ll
not use the ultrasound, I�ve got really sensitive fingers and can tell if
it�s a 3, 4 or 5 week pregnancy.
I�ll
not do the post op ultrasound, it has to be rolled in from the other room and
that�s just too much trouble. If
I don�t see pregnancy tissue then I�ll just bring her back in.
Those
hCG�s are just too expensive, I�ll just have her come back in a few days and
see if the pregnancy test is negative.
Do
not �gradually� introduce the protocol by doing only 4 and 5 week gestations
but not 3 week gestations. When a
woman with an undiagnosed ectopic pregnancy walks into your office, you have
incurred a liability for her care. The
best thing you can do to reduce your exposure is to see that she has a good
outcome. Telling her to return in a
week or two and giving her �ectopic precautions� will provide you with only
minimal protection if she has a bad outcome.
By doing the procedure and making the diagnosis you will have done her a
favor by making an early diagnosis.
The
protocol and algorithm have a great deal of redundancy.
This gives you a second chance when things go wrong.
Everyone makes the occasional mistake, when there is redundancy it is
necessary to make two mistakes in the same case to have a bad outcome.
Examples
of redundancy in the protocol:
You
document the disappearance of the uterine contents twice (ultrasound and in
examining POC)
When
you don�t see definite POC you document the disappearance
biochemically�don�t depend on pathologist seeing one villi
You
learn to correlate the amount of gestational tissue you see post op with the
ultrasound picture pre-op.
If
you have a lab that fails to do the pregnancy test right (false positive) you
quickly find out with your post-op b-hCG.
Other
benefits of early procedure:
Truly
minimizes the physiologic changes of pregnancy�no detectable change in
clotting factors, less time of exposure to high estrogen.
Stress
is known to be time related�someone who has been stressed for a week is more
likely to have physical and psychological reaction than someone who has been
stressed for a few days.
Sending
women away to return at a later date is costly and inconvenient for the woman.
Equipment
for Early Abortion:
Vaginal
ultrasound is essential for providing early abortions.
Curettes
can be ordered from :
Berkeley
Medevices (800)227-2388
Or
Cheshire
Medical Specialties
(800)243-3020
X-ray
view box (to lay flat on counter for POC viewing) or slide viewbox from
photography store. A small one
costs about $50.
A
small (3�) speculum:
Order
3� Graves or Moore-Graves
Also,
for wider opening you can use the Klopfer or Vu-More
MedGyn
Products
(800)451-9667
or
Cheshire
Medical
(800)243-3020
Film:
IPAS, PO Box 999, Camboro, NC, 27510
(800) 334-8446
 Summary: Steps in Protocol Summary: Steps in Protocol
1.
Do pre-operative sensitive pregnancy test
2.
Do pre-operative vaginal ultrasound
3.
Do counseling, informed consent and lab work (Rh status) as with any
abortion procedure
4.
Use short (3�) speculum
5.
Do procedure with hand held syringe (IPAS or Milex)
6.
Dilate cervix to 7 mm (#21 French with Pratt or Dennison dilator)
7.
Use 7 mm rigid cannula
8.
Do post-operative vaginal ultrasound to confirm removal of
sac and/or decidua
9.
Float tissue and examine with back lighting
10.
Order b-hCG
when chorionic membrane with villi not positively identified
11.
Repeat b-hCG in 24-72 hours in same
lab
 References References
[i]
Burnhill MS, Armstead JW. Reducing the morbidity of vacuum aspiration
abortion. Int J Gynaecol
Obstet 1978;16:204-209.
[ii]
Tietze C, Henshaw
SK. Percent of abortions with complications by gestation. In: Induced
Abortion: A World Review, 1986. New York: The Alan Guttmacher Institute,
1986:103.
[iii]
Carson SA, Buster JE. Ectopic pregnancy: Evolution of a surgical disease. N
Engl J Med 1993;329:1174-1181.
[iv]
Lenton AE, Neal LM, Sulaiman R. Plasma concentrations of human chorionic
gonadotropin from the time of implantation until the second week of
pregnancy. Fertil Steril 1982;37:773-778
[v]
Warren WB, Timor-Tritsch
1, Peisner D, Raju S, Rosen M. Dating the early pregnancy by sequential
appearance of embryonic structures. Am
J Obstet Gynecol 1989;161:747-53.
[vi]
Edwards J, Carson
SA, New Technologies permit safe abortion at less than six weeks�
gestation and provide timely detection of ectopic gestation. Am J Obstet
Gynecol 1997;176 1101-6
[i]
Kadar N, DeVre G, Romero
R. Discriminatory hCG zone: its use in sonographic evaluation for ectopic
pregnancy. Obstet Gynecol 1981;58:156-61.
[ii]
Bernaschek G,
Rudelsorfer R, Csaicsich P. Vaginal sonography versus serum human chorionic
gonadotropin in early detection of pregnancy. Am J Obstet Gynecol
1988;158:608-12.
[iii]
Goldstein S, Danon M,
Watson C. An Updated Protocol for Abortion Surveillance With Ultrasound and
Immediate Pathology. Obstet Gynecol 1994;83:55-8.
[iv]
Creinin MD, Washington AE. Cost of ectopic pregnancy management: surgery vs.
methotrexate. Fertil Steril 1993; 60:963-9.
|


![]()